Correlates of Serum Oxytocin Level and Semen Profile in Male Patients
Chitme HR, Azawi EA, Al Harthy AMS, Al Hinae MSS, Al Shuraiqi MZM, Al Salhi ASN and Al Balushi LAS
DOI10.21767/2471-9803.1000146
1Al Bushra Medical Multispecialty Complex, Muscat, Sultanate of Oman
2Oman Medical College, Bowshar Campus, Muscat, Sultanate of Oman
- *Corresponding Author:
- Chitme HR
Oman Medical College
Post Box 620, Baushar Campus
Muscat, Sultanate of Oman
Tel: +968-24504608
E-mail: hrchitme@gmail.com
Received date: February 03, 2017; Accepted date: March 08, 2017; Published date: March 18, 2017
Citation: Azawi EA, Chitme HR, Al Harthy AMS, Al Hinae MSS, Al Shuraiqi MZM, et al. Correlates of Serum Oxytocin Level and Semen Profile in Male Patients. Crit Care Obst Gyne. 2017, 3:2. doi: 10.21767/2471-9803.1000146
Copyright: © 2017 Azawi EA, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Central and peripheral level of oxytocin is found to be almost in the same level in both male and female however its direct relationship to male infertility is not yet studied clinically. Case control study was carried out to comparatively analyze serum oxytocin level and semen profile. Study was carried out among 60 patients including equal number of infertile case with age matching control. Serum oxytocin was measured by using ELISA tests and semen profiling was done by following routine methods of evaluation. The quantitative method involves comparison of factors between case and control. Results were analyzed by Pearson correlation and linear regression models to derive conclusion. The p value less than 0.05 was considered as significant. In our study 86.67% of the patients were diagnosed with primary infertility. About 90% of the patients were noted with 2-4 mL of semen. In this study serum oxytocin level in infertile patient is significantly (p<0.05) lower than compared to control patients. It is also found that infertile patients have significantly (p<0.01) lower sperm concentration, sperms with normal morphology, motile sperms and higher number of abnormally structured sperm cells compared to fertile group of patients. Comparative Pearson’s correlation analysis shown significant (p<0.05) correlation between serum oxytocin level and semen volume, sperm concentration and motility. We conclude from this study that serum oxytocin significantly lower in infertile patients and affecting fertility by affecting the semen volume, sperm motility and morphology.
Keywords
Oxytocin; Male infertility; Semen profile; Infertility; Sperm morphology; Oman
Introduction
Oxytocin, the neurohypophyseal nanopeptide is also known as ‘Love hormone’ recognized most commonly for its hormonal role in lactation and parturition despite of its equal amounts presence in both females and males. The actions of oxytocin range from the modulation of neuroendocrine reflexes to the establishment of complex social and bonding behaviors related to the reproduction and care of the offspring. It’s central and peripheral actions are mediated through ‘OT’ receptors [1]. A huge body of experimental evidence suggests that oxytocin facilitates both anticipatory and consummatory sexual behavior of male and females. Consummatory phase of the male sexual response includes penile erection, seminal emission and ejaculation, these responses are preceded by an anticipatory phase, which includes motivation towards and searching of an adequate partner for copulation [2]. The central oxytocinergic mechanism is proposed to involve dopaminergic reward pathways in the context of romantic partner relationships, dating, positive memories, supportive partner, cohabiting or marital relationship, marriage quality, physically affectionate contact, degree of partner’s understanding and appreciation and women’s ability to open up to them and interpersonal distress [3-4].
In male genital organs it is identified in the testis, prostate gland, epididymis, leydig cells and involved in the synthesis of testosterone, regulation of somniferous tubule contractility and modulation of steroidogensis [1]. Receptors in these organs are found to involve facilitation of sperm transport during the ejaculatory process [5]. Proerectile effect of oxytocin is mediated by dopamine agonists, excitatory amino acids, nitric oxide donors and other substances such as hexarelin analogue peptides and VGF-derived peptides [6,7]. Recently concluded study shown a dramatic improvement in libido, erection, climax and orgasm by intranasal oxytocin administration in a patient having difficulties such as social avoidance and relational problems [8,9].
Over the past decade the central actions of oxytocin is believed to reduce corticosterone cortisone level, and increases CCK level secretion to counteract the stress and tension associated reduction in sperm count, motility, and morphological defects causing idiopathic infertility in male [10,11]. Oxytocin is also involved in aggressiveness, fear, curiosity, anxiety, and stress by acting through its receptors [12].
Involvement of oxytocin in male primary and secondary sexual growth is clearly seen in multiple studies. However, its direct relationship to male infertility is not yet studied clinically. Thus, whether oxytocin may really facilitate sexual behavior in humans and useful in male infertility treatment is still far from being ascertained. It has to be hoped that this study will reopen the research aimed at the role of oxytocin by which it controls male sexual activities and fertility in order to improve the actual knowledge of the physiology of such functions and the quality of life of people suffering for these dysfunctions as well. Understanding the level of oxytocin in infertile male patients will help to develop new therapeutic strategies for male infertility related sexual dysfunctions and new opportunities for male contraception. This study will also need of academic and scientific community to know whether there is any relationship between the level of oxytocin and semen profile. Primary aim of the study was to estimate and compare the serum oxytocin level in male fertile and infertile Omani patients and to correlate its level to the semen profile associated with male infertility.
Research Methodology
Study design
It is case control study carried out at Al Bushra Medical Multispecialty Complex, Muscat for six months period.
Selection of participants
Criteria of Inclusion in fertile group were those who meet the standard definition of male infertility, visiting study centre, volunteered to involve in the study, aged 20-50 years and infertility not due to vasectomy. The group of fertile patients considered as control in this were those who are diagnosed with infertility only due to female factors and matching age group. The criteria of exclusion included those who have a history of using contraceptives from past one year, female partner having history of chemical menopause and chemotherapy and participant not willing to involve in the study and not agreed to sign the written consent form.
Research instrument
As per the hospital record about 250 male infertile patients visit study centre per year. In consideration of α and β levels at 0.01 and correlation coefficient of 0.6 the sample size was calculated to be 53. Therefore, in this pilot study we considered 60 patients visiting study centre and meeting above inclusion and exclusion criteria. Male patients who are diagnosed with male infertility during study period go through two separate phases of study. In the first phase of study, required information was obtained from case files and in second phase blood sample was obtained for oxytocin level measurement.
Oxytocin enzyme immunoassay
This assay was carried out by Enzyme immunoassay method using Oxytocin Assay kit purchased from Wuhan Fine Biotech Co. Ltd. Wuhan, China. The procedure provided by the supplier was followed in estimation of serum oxytocin. In brief, includes standards or diluted samples was pipetted into the provided microtiter plate coated with an antibody to capture antibodies. An oxytocin peroxidase conjugate was added to the standards and samples in the wells. The binding reaction was initiated by the addition of a polyclonal antibody to oxytocin to each well. After an incubation the plate was washed and substrate was added. The TMB substrate reacts with the bound oxytocin peroxidase conjugate to produce a yellow colored product read at 450 nm. The intensity of the generated signal was detected in a microtiter plate reader [13].
Medical ethics
The study is approved by Institutional Ethics Committee of Oman Medical College and the study centre. Identity of the participants and findings was treated with highest possible degree of confidentiality. Participants were clearly explained the purpose of the study and their written consent to take part in this study was sought prior to their inclusion. Participation in this study was voluntary and participants have the right to withdraw at any period of the investigation. Team member along with a nurse belonged to the respective hospital carried out collection of data. Information collected from the hospital and the patient remain confidential. All unused specimens were sensibly disposed according to the biosafety and medical guidelines followed at clinic.
Statistical analysis
Each case were given a case number and the information collected in this study entered directly into SPSS version 19 and analyzed using descriptive statistics such as mean and standard deviation for continuous numerical data, and for demographic and other categorical data percentage-frequency distribution were used and compared using chi-square tests. Correlations between oxytocin and other fertility factors were estimated using Pearson correlation analysis. The confidence intervals (CI) of infertility were obtained by fitting a multiple regression analysis. Any difference in continuous variables of control and case group were analysed by Students t test. A p value of less than 0.05 were considered statistically significant.
Result
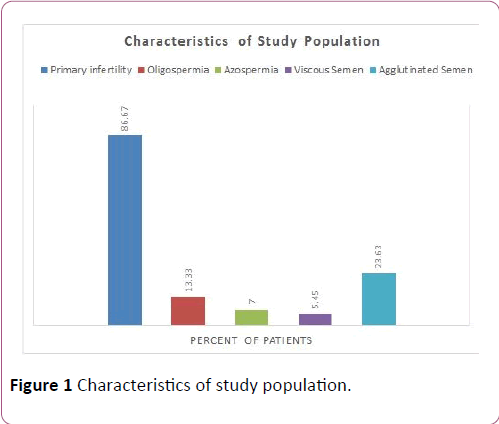
Characteristics of study population
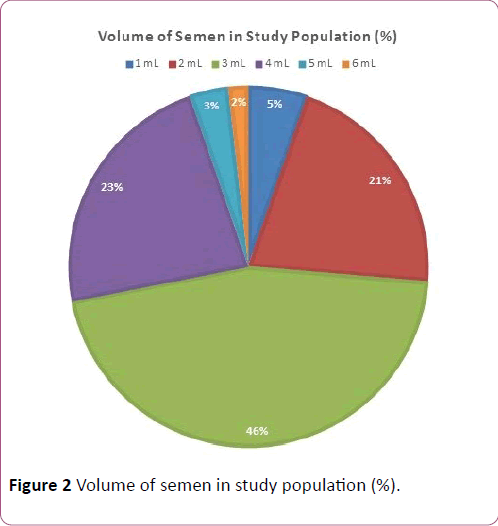
In this study 86.67% of the patients were having primary infertility and 13.33% were diagnosed with secondary infertility. It is also noted that 13.33% were oligospermic, 7% were azoospermic, 5.43% were with thick and viscous semen and 23.63% of them were known to have agglutinated semen Figure 1. As presented in Figure 2 volume of semen was varying in patients involved in the study. Most of the patients (46%) were noted with 3 mL whereas 23% of them were with 4 mL and 21% of them were with 2 mL of semen.
Comparative analysis of serum oxytocin and semen profile
Results in Tables 1 and 2 shows a significant difference in semen profile and serum oxytocin in fertile and infertile patients. Serum oxytocin level in infertile patient is significantly (p<0.05) lower (13.83 ± 4.15) than to control patients (19.04 ± 10.95) with a confidence interval of 0.93 to 9.49 (CI 95%). It is also found that infertile patients have significantly (p<0.01) lower sperm concentration 31.22 ± 2.48 million/mL compared to 88.48 ± 8.45 million/mL (21.16 to 92.95, CI 95%). Highly significant (p<0.001) normally structured 15.58 ± 9.16% sperm cells compared 26.55 ± 6.96% and abnormally structured sperm cells were 84.33 ± 9.49% in infertile compared to 73.45 ± 6.96% of fertile male. Motility of sperm cells in infertile patients 34.78 ± 17.02% was very significantly (p<0.001) lower compared to 53.79 ± 9.6% compared to control group of patients with confidence interval of 11.5 to 26.51 (CI 95%).
| Factors | Case | Control | Level of Significance | 95% Confidence Interval of the Difference | |
| Lower limit | Upper limit | ||||
| Semen volume (mL) | 3.02 ± 0.17 | 3.07±0.19 | 0.84 | -0.47 | 0.57 |
| Semen pH | 7.233 ±0.03 | 7.23 ± 0.03 | 0.95 | -0.09 | 0.09 |
| Sperm concentration (million/mL) | 30.25 ± 5.18 | 88.28 ± 15.69 | 0.001*** | 24.92 | 91.13 |
| Normal sperm morphology (%) | 12.99 ± 1.9 | 26.55 ± 1.29 | 0.001*** | 9.05 | 18.26 |
| Abnormal sperm morphology (%) | 69.79 ± 6.23 | 73.45 ± 1.29 | 0.57 | -9.09 | 16.39 |
| Sperm motility | 28.57 ± 3.87 | 53.79 ± 1.78 | 0.001*** | 16.77 | 33.67 |
| Oxytocin level | 2.61 ± 0.2 | 5.9550 ± 1.93 | 0.09 | -0.53 | 7.22 |
| ***P<0.001 by student’s 2 tailed test | |||||
Table 1: Comparative Analysis of Fertility Factors in Case and Control Group of Population.
| Factors | Total/ Infertile | Coefficients | F | df | P Value | Pearson Correlation | |
| Semen volume (mL) | Total | 6.153 | 3421.26 | 0.099 | 55 | 0.754 | -0.042 |
| Case | 0.371 | 33.299 | 0.29 | 27 | 0.595 | 0.337 | |
| Semen pH | Total | 4.307 | 3402.24 | 0.065 | 51 | 0.4 | -0.036 |
| Case | 0.043 | 34.287 | 0.031 | 26 | 0.861 | 0.674 | |
| Sperm concentration | Total | 0.247 | 3427.8 | 0.004 | 56 | 0.475 | 0.008 |
| Case | 0.543 | 34.08 | 0.43 | 28 | 0.517 | 0.126 | |
| % Sperms with normal morphology | Total | 102.48 | 3325.57 | 1.726 | 56 | 0.097 | 0.173 |
| Case | 1.253 | 33.37 | 1.014 | 28 | 0.323 | 0.226 | |
| % Sperms with abnormal morphology | Total | 2.651 | 3425.39 | 0.043 | 56 | 0.418 | -0.028 |
| Case | 2.254 | 32.369 | 1.88 | 28 | 0.182 | 0.416 | |
| Sperm motility | Total | 46.204 | 3374.09 | 0.753 | 55 | 0.195 | 0.116 |
| Case | 4.576 | 28.99 | 4.104 | 27 | 0.053* | 0.337 | |
| A simple linear regression predicted a significant *p<0.05 correlation between serum Oxytocin level and fertility factors | |||||||
Table 2: Correlation Analysis of Serum Oxytocin and Semen Profile in Study Population.
Correlation analysis of serum oxytocin level and semen profile
Comparative Pearson’s correlation analysis and linear regression analysis shown an insignificant correlation between serum oxytocin level and most of the semen factors except the semen volume. In this study, serum oxytocin level in total population is negatively correlated with semen volume (-0.154), semen pH (-0.064) and abnormal sperm morphology (-0.214) whereas positively correlated with normal sperm morphology (0.219), sperm concentration (0.125) and sperm motility (0.12). We observed significant (p<0.05) Pearson correlation only between serum oxytocin level and semen volume in control group of patients but not in total population and infertile group of patients. Pearson correlation and Spearman correlation have both shown a positive correlation between serum oxytocin level and normal sperm morphology and negative correlation with abnormal sperm morphology. A simple linear regression was calculated to predict serum oxytocin level based on semen profile. Significant regression equation (-0.322) was found between serum oxytocin (F (4.576, 28.99))=4.104, p<0.05), R2 of 0.136 with sperm motility in infertile male only. The correlation table shows a positive correlation of serum oxytocin, semen volume, sperm concentration, normal and abnormal morphology along with sperm motility respectively in infertile patients.
As we have already seen a coefficient of 0.674 suggests there is a strong positive relationship between serum oxytocin and semen volume in infertile patients while r2=0.454 suggests that 45.4% of the variance in serum oxytocin concentration can be explained by the semen volume. Finally the t-test in the table tells us that sperm concentration is making a statistically significant (p<0.05) contribution to the predictive value of the study.
Discussion
Very recently it was observed that 24 IU nasal dose of oxytocin modulated brain reward system in men and promoted attraction in both known and unknown partners [14]. Present study was a case-control study to correlate the serum Oxytocin level in male infertile Omani patients and to its level to the factors associated with male infertility. The study was carried out at Al Bushra Medical Multispecialty Complex, Muscat. We studied many male infertility factors such as semen volume, semen pH, sperm concentration, normal & abnormal sperm morphology, sperm motility, semen viscosity, normal & abnormal time of liquefaction in relation with serum Oxytocin level.
The oxytocin and its receptor regulate reproductive physiology and sociosexual behaviors [15]. One of the study has proven that oxytocin might have a role in the ejaculatory process, stimulating sperm release from the epididymal storage [16]. In our study the serum oxytocin level in group of infertile patients was lower than the control along with lower semen volume, sperm concentration, normal morphology of sperm cells and sperm motility. These results substantiates earlier study which has shown pulse systemic oxytocin appears to be associated with ejaculation. It is appear to have an autocrine paracrine role be involved in contractility of the seminiferous tubules [17]. Our study also endorses past study which has observed no obvious correlation between plasma oxytocin levels and sperm count, sperm motility or the number of abnormal forms [18].
It is known from previous studies that male genital organs testis, epididymis and leydig cells are innervated by oxytocinergic mechanism and involved in spermatogenesis and modulate androgen levels in these tissues via stimulation of the conversion of testosterone to dihydrotestostone by 5-alphareductase1, 5 Exogenous administration of oxytocin has, in some cases, been shown to increase the numbers of ejaculated sperm, possibly by stimulating contractions of the reproductive tract and thus aiding sperm passage [19]. In our study most of the semen factors have correlation to some extent with serum oxytocin but not significant supporting earlier experiment based study which has illustrated that sexual stimulation increase plasma concentrations of oxytocin but not vice versa [20]. Results of our study indicate that serum oxytocin level in infertile patient is low thereby affecting the spermatogenesis and leading to lower semen volume and sperm concentration than the fertile control patients. We also found a significant correlation between normal sperm morphology, sperm concentration, semen volume and serum oxytocin level. Substantiating the earlier study which believed to reduce cortisone level and increase CCK level to counteract the stress and tension thereby maintaining normal morphology of sperms [10,11].
There’s a significant linear relationship between the level of serum Oxytocin and sperm motility in infertile patients [10,11]. Increase in serum oxytocin level has higher level of correlation with sperm morphology and normal sperm morphology is an important factor to determine sperm motility. Therefore, our study shows the deficiency of oxytocin in infertile patient is probably the cause for abnormal morphology and immotile sperms. Our results supports the study carried out to correlate seminal oxytocin level and sperm count, sperm motility, and sperm abnormal forms [21].
Lui, et al. [22], investigated the relationship between oxytocin and oxytocin receptor gene expression in both fertile and infertile men. This study was involving obstructive azoospermia, idiopathic asthozoospermia, idiopathic oligozoospermia and healthy patients. Serum oxytocin level in our study was lower in infertile group than in fertile group contradicting the study [22]. It is to underline here that this study has not stratified the patients based on the characteristics considered by Lui et al. Since we have not considered the level of serum LH, FSH, testosterone and expression of oxytocin receptors therefore the results of our study are incomparable with this study. However, they concluded that there is a significant difference in oxytocin concentration and expression of oxytocin receptor gene expressions between infertile and fertile men indicating linkage of oxytocinergic system in male fertility similar to our study [22]. Since, there is a correlation between level of serum oxytocin and semen profile it is important for all healthcare professionals including psychiatrist, endocrinologist, gynaecologist, infertility specialist and nursing staff to provide a comprehensive care to improve ability of a male infertile patient to conceive a child [23].
Conclusion
Based on the results of our study we conclude that the serum oxytocin level is significantly less in infertile group of male patients. These results indicate that there is a relation between serum oxytocin level and seminal properties such as sperm concentration, sperm morphology and sperm motility. However, we recommend further detailed and extensive studies by involving more patients, hospitals and multiple centres for further confirmation and support the results of this study.
Acknowledgment
We would to thank clinical, technicians, nursing and administrative staff of Al Bushra Medical Multispecialty Complex, Muscat for their time and assistance in completing this study.
Declaration of Interests
We declare that there is no conflict of interest that could be perceived as prejudicing the impartiality of the research reported.
References
- Hiremath GS, Chitme HR (2009) Possible Central Role of Oxytocin in Neurobehaviour of Male Rats and Mice. Advances in Environmental Biology 3: 84-91.
- Argiolas A, Melis MR (2013) Neuropeptides and central control of sexual behaviour from the past to the present: a review. ProgNeurobiol 108: 80-107.
- Campbell A (2008) Attachment, aggression and affiliation: The role of oxytocin in female social behaviour. Biological Psychology 77: 1-10.
- Scheele D, Striepens N, Güntürkün O, Deutschländer S, et al. (2012) Oxytocin modulates social distance between males and females. J Neurosci 32: 16074-16079.
- Filippi S, Vannelli GB, Granchi S, Luconi M, et al. (2002) Identification, localization and functional activity of oxytocin receptors in epididymis. Mol Cell Endocrinol 193: 89-100.
- Gil M, Bhatt R, Picotte KB, Hull EM (2011) Oxytocin in the medial preoptic area facilitates male sexual behavior in the rat. HormBehav 59: 435-443.
- Argiolas A, Melis MR (2005) Central control of penile erection: role of the paraventricular nucleus of the hypothalamus. ProgNeurobiol 76: 1-21.
- Macdonald K, Feifel D (2012) Oxytocin in schizophrenia: a review of evidence for its therapeutic effects. ActaNeuropsychiatr 24: 130-46.
- Heiman JR, Long JS, Smith SN, Fisher WA, et al. (2011) Sexual satisfaction and relationship happiness in midlife and older couples in five countries. Arch Sex Behav 40: 741-753.
- Márquez S, Villaseñor RM, Rojas L, Aragón-Martínez A, Torres GR (2014) Sexual behavior attenuates the effects of chronic stress in body weight, testes, sexual accessory glands, and plasma testosterone in male rats. HormBehav 66: 766-778.
- Lunstad J, Birmingham WA, Light KC (2008) Influence of a "warm touch" support enhancement intervention among married couples on ambulatory blood pressure, oxytocin, alpha amylase, and cortisol. Psychosom Med 70: 976-985.
- Mak P, Broussard C, Vacy K, Broadbear JH (2012) Modulation of anxiety behavior in the elevated plus maze using peptidic oxytocin and vasopressin receptor ligands in the rat. J Psychopharmacol 26: 532-542.
- Wuhan City (2016) Human OT (Oxytocin) ELISA Kit.
- Scheele D, Plota J, Wagner B, Maier W and Hurlemann R (2016) Hormonal contraceptives suppress oxytocin-induced brain reward responses to the partner’s face. SocCogn Affect Neurosci 11: 767-774.
- Takayanagi Y, Yoshida M, Bielsky IF, Ross HE, et al. (2005) Pervasive social deficits, but normal parturition, in oxytocin receptor-deficient mice. ProcNatlAcadSci 102: 16096-16101.
- Filippi S, Vannelli GB, Granchi S, Luconi M, et al. (2002) Identification, localization and functional activity of oxytocin receptors in epididymis. Mol Cell Endocrinol 193: 89-100.
- Ivell R, Balvers M, Rust W, Bathgate R, and Einspanier A (1997) Oxytocin and male reproductive function. AdvExp Med Biol 424: 253-264.
- Ogawa S, Kudo S, Kitsunai Y, Fukuchi S (1980) Increase in oxytocin secretion at ejaculation in male. ClinEndocrinol 13: 95-97.
- Thackare H, Nicholson HD, Whittington K (2006) Oxytocin-its role in male reproduction and new potential therapeutic uses. Hum Reprod Update 12: 437-448.
- Veronesi MC, Tosi U, Villani M, Govoni N, et al. (2010) Oxytocin, vasopressin, prostaglandin F(2alpha), luteinizing hormone, testosterone, estrone sulfate, and cortisol plasma concentrations after sexual stimulation in stallions. Theriogenology 73: 460-467.
- Mostafa T, Rashed LA, Osman I, Marawan M (2015) Seminal plasma oxytocin and oxidative stress levels in infertile men with varicocele. Andrologia 47: 209-213.
- Lui C, Cui XG, Wang YW, You ZD, Xu DF (2010) Association between neuropeptide oxytocin and male infertility. J Assist Reprod Genet 27: 525-531.
- Ciccone MM, Aquilino A, Cortese F, Scicchitano P, et al. Feasibility and effectiveness of a disease and care management model in the primary health care system for patients with heart failure and diabetes (Project Leonardo). Vasc Health Risk Manag 6: 297-305.
Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences